Harder & Mehl
Periodontitis
Do your gums start bleeding when you are brushing your teeth or when you are eating? Might your gums already have started retreating? Then you are highly likely to be suffering from periodontitis. Around 80 per cent of the German population are suffering from parodontosis – as periodontitis is commonly known.
The most common gum disease for adults is the periodontitis. Plaque and bacteria attack the gums, and the gum in the affected area pulls back and becomes inflamed. It can lead to tooth loss and potential damage to other internal organs (heart, lungs), diabetis difficult to control, early onset of Alzheimer's disease or even lower birth weight.
Very often those affected by this condition do not even realise that something might be wrong with their gums. This is because gingivitis often goes unnoticed, and it is pain-free. However, the consequences may be severe: Gum withdrawal, bone loss or an increased risk of a stroke or heart attack.
At our Dental Clinic we offer your not just periodontosis therapy, but also quick diagnosis and careful as well as thorough treatment. First of all inflammations in your mouth cavity are removed. We then proceed to a targeted treatment of individual, remaining gum pockets.
In our periodontitis treatment we place great importance on long-term care. Our structured recall system is part of this. This system ensures that patients come in for regular check-ups. This ensures successful long-term treatment.
We will be more than happy to personally assist you should you have any queries at all.
FAQ
Periodontitis refers to the inflammation of the gums and the periodontium as a whole – along with tooth decay it is the most widely spread dental condition. Periodontitis attacks the tissue that holds the teeth in place. With this condition not being accompanied by any pain at all, it often goes unnoticed for a long time.
The risk of contracting periodontitis increases with age. If left untreated, periodontitis can result in untimely loss of your teeth. The chronical inflammation of the periodontium tends to occur in phases.
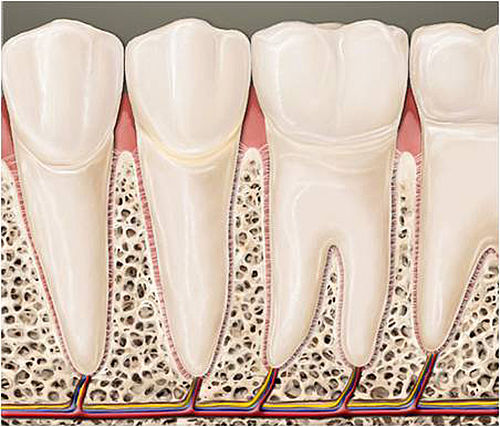
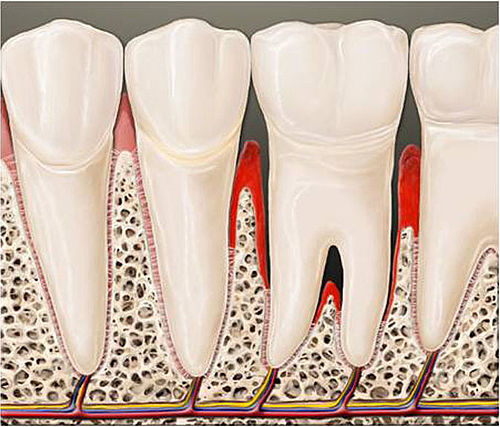
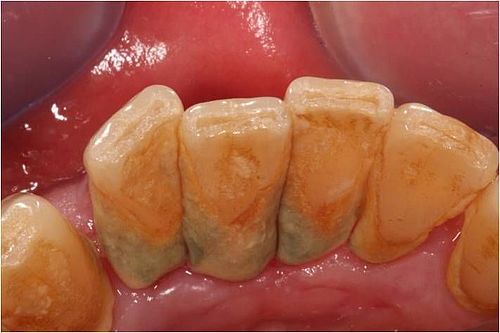
Without plaque there is no periodontitis. Plaque that settles on the surface of the tooth, most frequently in interdental spaces, consists of a network of bacteria. The oral cavity is home to well over 600 different types of bacteria, most of which pose not threat to your oral health. They form what is termed a biofilm – meaning plaque – on the surfaces of your teeth, the edge of your gum and interdental spaces. If plaque is not thoroughly and regularly removed, it hardens, and it forms dental calculus. Bacterial metabolites cause inflammation in the gums, also known as gingivitis. The main symptom of gingivitis and the first warning signal is bleeding gums.
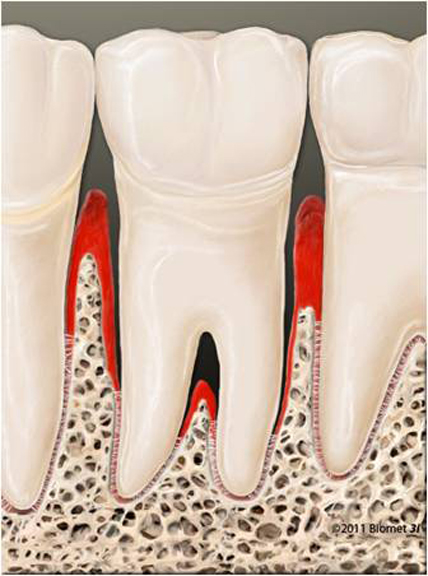
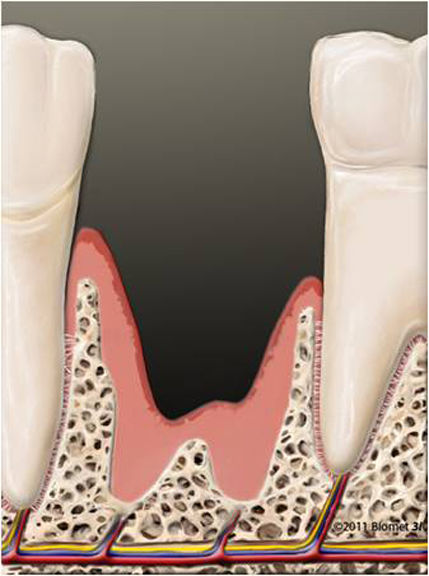
The area in which the gums meet the tooth forms a natural barrier. This barrier can often prevent bacteria from getting deeper into the gums. If this condition is left untreated, however, this protective wall becomes penetrable, and the inflammation can spread to the bone and the periodontal ligament. What is next is the staged destruction of the tooth-bearing peridentium. The gums dissipate, and part of the remaining peridentium dissipates. Next what is called pockets forms. From this moment on yet more bacteria can enter. The body's own immune defences cause dissipation of the periodontium following the bacterial attack. The gums retreat, and so do the jaw bones. The tooth become loose. In the worst of cases your teeth might fall out – even without ever having been affected by tooth decay or without you ever having had a filling.
Not every person is equally at risk of being affected by periodontitis. So, too, the process and the severity of the condition are dependent upon certain internal and external factors. The latter affect our immune system.
- It has been scientifically proven that disposition to periodontitis might be passed down from generation to generation.
- Insufficient oral hygiene is the main contributor to the formation of periodontitis. As mentioned above dental calculus and bacterial deposition cause gingivitis.
- Nicotine consumption has an adverse effect on our immune system. This means that smokers are twice to seven times more likely to suffer from gingivitis. Moreover smokers often do not know that they have gingivitis because the first warning signal – bleeding gums – often does not occur in them. The likelihood of success is limited if the patient keeps smoking. The first and most effective measure you can take is this: Stop smoking immediately!
- Diabetes increases the risk of patients to be affected by periodontitis. Badly adjusted blood sugar values immediately impact on the immune systems of the periodontium. This means that gum inflammation may occur more frequently, and they may take longer to heal.
- Psychological stress and hormonal changes also impact on the immune system. Periodontitis is more likely to occur, and it may develop more quickly. During pregnancy there is also an increased risk of contracting periodontitis.
- Inherent or acquired weaknesses in the immune system, such as AIDS, are a contributing factor to patients developing periodontitis.
- Certain medication, such as medication aimed at reducing a patient’s blood pressure or other drugs that may weaken the immune system, can cause your gums to swell. This may be a contributing factor in the development of periodontitis.
The inflammatory substances of the bacteria can enter our blood circle by way of the inflamed tissue in the periodontium. This way these substances can be transported to other parts of the body.
Diabetes
There is negative interaction between periodontitis and diabetes. If your glucose values are badly adjusted, this may be a contributing factor in developing periodontitis. This also works the other around. Periodontitis makes it harder to adjust your blood sugar levels. This is because the effectiveness of the insulin used in diabetes treatment is weakened due to gingivitis.
Strokes and heart attacks
The bacteria in your oral cavity and their inflammatory by-products influenced the clogging of the arteries negatively. In periodontitis patients that is an increased risk of strokes and heart attacks. Moreover bacteria absorbed into the blood circle by way of the periodontal gap can be a contributing factor to endocarditis, artificial heart valves as well as hip and knee joints.
Pregnancy
Pregnant women tend to be more susceptible to gingivitis and periodontal inflammation. A severe form of periodontitis can even increase the risk of complications during pregnancy and of underweight in the newborn sevenfold.
Despite the fact the periodontitis may go unnoticed due to the fact that it is painless in its early stages, there are still warning signs that may point to an inflammation of the periodontium:
- Bleeding gums (when brushing your teeth or when eating)
- Swollen and red gums
- Retreating gums
- Sensitive tooth necks
- Lasting bad breath and/or continuously bad taste in your mouth
- Pus exiting the gingival pockets
- Loosening teeth
If you have noticed one or more of these warning signs, you should see a dentist immediately. Only a specialist can tell you whether or not you have periodontitis.
First of all we evaluate the level of severity of your condition. We take a large-scale X-ray (OPG) to better see the formation of your jaw bone. We also measure the depth of pockets with rounded probes with scaling. The level of bleeding, loosening of the teeth as well as other factors are determined. If your periodontitis is severe or aggressive in nature it may be that we may have to prescribe antibiotics. For this purpose we will do a bacteria test. Its results are evaluated at our laboratory. This allows us to determine which type of antibiotics would be best in your case.
The treatment requires that the dental surfaces be free from plaque and that the patient have good oral hygiene. Only then can the treatment successful in the long term.
This is why, prior to commencing treatment, one or two appointments with our dental hygienist may be necessary. Our professional dental cleaning is the perfect preparation for this treatment: Initially all the visible areas of your teeth our cleaned thoroughly. By analysing your teeth we can determined how you can best care for them at home.
This is when periodontitis treatment can commence.
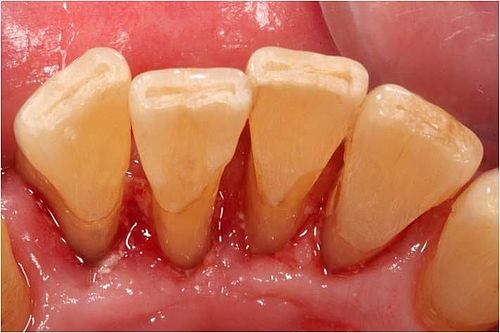
We start by cleaning the pockets, using hand tools. This is done under local anaesthesia. This treatment tends to be ultrasound aided. This allows us to smoothen the root surfaces. This makes it more difficult for bacteria to deposit in those areas.
Following treatment it takes about two to three days for your gums to recover from this treatment. During this period the inflammatory swelling of your gums will go down – meaning that your gums will again be tightly and strongly aligned with the necks of your teeth. However, this also means that your gums will shrink ever so slightly.
During the first few weeks after treatment the necks of your tooth may be sensitive as a result.
We will check the result over the course of the next few weeks. In most cases gingivitis is reduced following this initial treatment. Should treatment not have been successful or should the pockets be particularly deep in your case, surgery may be required.
During follow-up treatment we will then clean the root surfaces of your teeth. To achieve this we will open your gums. Cleaning will be done using hand tools as well as ultrasound just like before. Again, this is done while you are under local anaesthesia. This allows us to better recognise and remove gaps, deep-rooted depositions and unevennesses.
Periodontitis usually leads to gum recession, in severe cases even to the degradation of the root cementum and the bony tooth compartment in the jaw (so-called alveolar bone). In addition, the collagen fiber bundles in the connective tissue, which connect the root cementum with the bone are destroyed. All this can lead to tooth loss. Thanks to the guided tissue regeneration (GTR) and surgical gum corrections, we can save the teeth of our patients and help them to retain a great smile.
GTR (Guided Tissue Generation) refers to procedure that serves the purpose of restoring the tissue of your periodontium. The latter may have become degenerated due to usually severe and aggressive periodontitis. GTR is necessary because the different types of tissues that make up the periodontium do not all recover at the same speed. The gums are intended to close wounds. This means that gums tend to grow much faster than the root element, the collagen fibre bundles or the alveolar bone. However, it is exactly these that ensure that your teeth are securely kept in place. This is where GTR comes into play: This procedure stimulates regeneration of these types of tissue, and it keep the gums from spreading uncontrolled. If this were to happen, it could result in a disruption of the healing process of the remaining periodontium.
Following local anaesthesia of the area to be treated, we proceed to opening the gums. Only a small cut is needed for this. This reveals the surface of the root. We start off by removing depositions such as plaque or dental calculus. Should craters have already formed in the alveolar bone, we will fill these with bone substitute. This tends to be granulated. The bone material uses this granulate as a guide rail. On the other hand the material functions as a type of building material.
We then cover the area opened and treated with a membrane. This allows for the creation of a barrier between the gums and the dental root as well as the bone tissue. The cavity created this way allows the collagen tissue fibres and the bone tissue to regenerate freely – the bone tissue is then regenerated.
The membrane does not need to be removed later on. This is because we exclusively use absorbable membranes. The last step is to stitch the area opened.
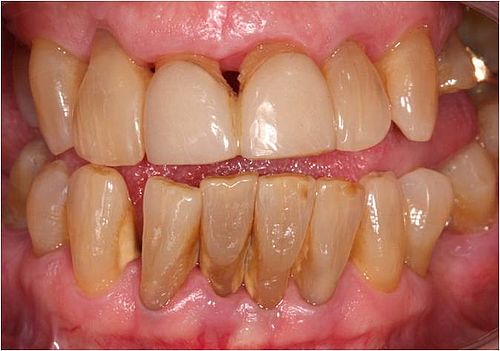
Periodontitis often results in retreating gums. This results in exposed necks of the tooth. These then tend to be extremely sensitive to cold, heat, sweetness and sourness. In addition there is usually an aesthetic issue as well: especially with the visible front teeth. These can seem unusually long as a result. A lot of patients then tend to avoid an open and unrestrained smile. Plastic-aesthetic gum correction helps you achieve better quality of life and more self-confidence – because it regenerates the gums.
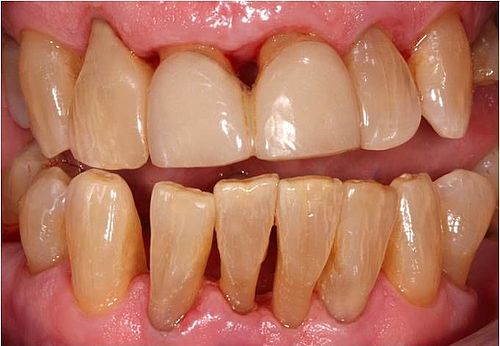
In this procedure exposed root surfaces are covered in gum again in a micro surgical plastic procedure. In this procedure tissue from your palate may be transplanted onto the exposed tooth necks. Alternatively existing gum material may be loosened and stretched until the areas exposed have been covered.
Following an in-depth conversation discussing your options we will decide together which method may be best suited for you individually.
A large part of the cost involved in these treatments may in some cases be paid by your statutory health care provider. Unfortunately statutory health care providers do not cover all the treatments options that modern dentistry has to offer. In the event that there may be costs to be borne by yourself, we will, of course, discuss this in detail prior to your treatment.
Now it is your turn! Periodontitis is a chronical disease. This means that you have to be consistent in your aftercare. This is to keep active periodontitis and additional bone loss from returning. It also helps prevent premature loss of your teeth.
This consists of the following three aspects:
- excellent oral hygiene at home
- have your teeth cleaned professionally between two or four times a year
- regular check-ups
Only by cooperating with us will you be guaranteed long-lasting effects of the treatment you have undergone. Without your cooperation there is a very high risk of periodontitis returning.
Why do I have gum disease and what can I do to prevent it?
Course of a periodontal disease of the periodontium (parodontitis)
Procedure of gum treatment
More Questions?
We answer commonly asked questions about tooth preservation in detail – and will gladly answer them in a personal consultation!
Your specialists for Tooth Preservation
Preventing Gum Disease Effectively
PD Dr. med. dent. Sönke Harder
“In order to prevent gum disease, regular dental check-ups, as well as professional tooth cleaning, are essential. This is the best way to remove tartar, giving periodontitis no chance.”

Fighting Gum Disease
Prof. Dr. med. dent. Christian Mehl
“Gum transplants can, for example, easily compensate for front teeth with different lengths and protect the periodontium from recession.”